Key Takeaways
- The American College of Radiology (ACR) permits virtual supervision for contrast administration when combined with on-site medical professionals trained in reaction management.
- CMS policies authorize real-time, two-way audio/video technology for remote oversight, with permanent authorization for diagnostic tests effective January 1, 2026.
- On-site training in patient assessment, emergency protocols, and medication administration remains mandatory for clinical safety and regulatory adherence.
- State and local compliance requirements often vary from national guidelines, necessitating rigorous documentation and regional awareness.
- Virtual supervision models optimize radiology department resources without compromising established safety protocols for patient care.
The Evolution of Contrast Administration Oversight
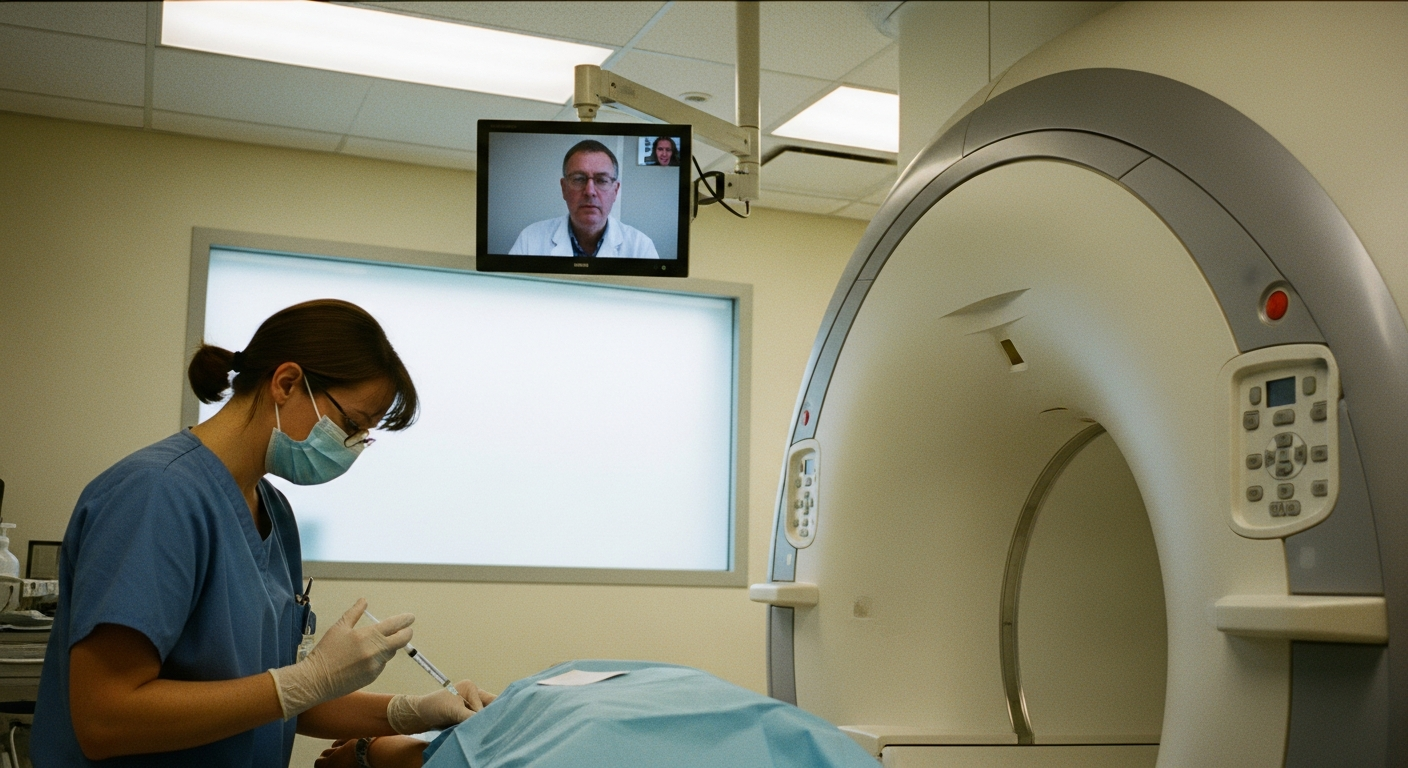
The methodology for supervising contrast administration has transitioned from a strict requirement for physical presence to a data-driven model that integrates remote physician oversight. This shift addresses the increasing volume of diagnostic imaging while maintaining clinical safety standards during contrast procedures. By leveraging telecommunication technology, facilities can maintain the “immediate availability” of a radiologist without requiring their physical presence in the office suite.
ACR Guidelines for Virtual Supervision
The American College of Radiology updated its contrast supervision guidelines in early 2024, introducing the flexibility for physicians to provide direct supervision remotely via real-time audio-video technology. This revised framework stipulates that when a physician provides direct supervision—whether on-site or virtually—a medical professional trained to manage contrast reactions must be physically present at the facility.
This approach recognizes the technological capabilities of modern healthcare systems while preserving a safety net for immediate physical intervention. The ACR’s guidance ensures that providers can utilize virtual oversight without degrading the response quality for adverse events. According to internal experts at ContrastConnect, understanding specific virtual contrast supervision metrics is essential for successful implementation.
Healthcare facilities adopting this model must ensure their workflows align with state and local regulations, as institutional policies often require more stringent response times than federal baselines. The flexibility provided by the ACR allows for improved resource allocation across multi-site organizations while upholding the rigorous safety standards required during intravascular contrast administration.
CMS Direct Supervision Policy and the 2026 Permanent Rule
The Centers for Medicare and Medicaid Services (CMS) has established a regulatory foundation for virtual direct supervision through real-time audio/video technology. While temporary flexibilities were introduced during the COVID-19 public health emergency, the Calendar Year 2026 Physician Fee Schedule has codified these changes into permanent policy for diagnostic tests.
Technical Communication Standards
CMS requirements specify that virtual direct supervision must involve real-time, two-way audio and video communication between the supervising physician and the location where services are rendered. Audio-only communication (such as telephone calls) does not meet the standard for “immediate availability.” The supervising physician must be able to observe the procedure, communicate with on-site staff, and intervene immediately through the technological interface.
To maintain clinical safety, the technical infrastructure must support high-fidelity transmission. Industry benchmarks suggest that platform latency exceeding 150 milliseconds is unacceptable, as any delay in communication can hinder the management of a rapidly escalating anaphylactic reaction. Facilities must invest in robust IT infrastructure with redundant communication pathways to ensure uninterrupted supervision during procedures.
Permanent Status for Diagnostic Tests
Effective January 1, 2026, CMS permanently authorized virtual direct supervision for diagnostic tests, including contrast-enhanced CT and MRI (under 42 CFR § 410.32). This permanent status provides healthcare administrators with the regulatory certainty needed to design long-term staffing models. Unlike other medical services that may face expiring flexibilities at the end of 2025, diagnostic imaging has a clear, permanent pathway for remote oversight.
On-Site Reaction Management Training Requirements
While virtual supervision provides operational flexibility, the presence of appropriately trained on-site staff is non-negotiable. The ACR’s 2024 update identifies specific qualifications that on-site medical professionals must possess. These individuals act as the “hands” of the remote supervising physician, executing immediate life-saving interventions before emergency medical services arrive.
1. Patient Assessment and Reaction Recognition
On-site staff must be trained to recognize the early signs of both physiologic and allergic-like contrast reactions. Training programs cover the spectrum of adverse events, from mild symptoms like localized hives or nausea to severe manifestations such as laryngeal edema, bronchospasm, and hypotensive shock.
Effective training typically involves simulation-based exercises that replicate the high-pressure environment of a contrast reaction. These simulations help medical professionals develop the clinical judgment necessary to differentiate between a vasovagal response and a true allergic reaction, ensuring that the remote radiologist receives accurate, real-time data during a consultation.
2. Emergency Response Protocols
Standardized response protocols provide a step-by-step framework for managing reactions based on severity. These protocols include:
- Immediate stabilization of the patient and cessation of contrast administration.
- Rapid notification of the virtual supervising physician through the dedicated audio/video interface.
- Activation of the facility’s internal emergency response team or local EMS for severe reactions.
- Implementation of the ACR Manual on Contrast Media treatment algorithms.
Staff members are trained to provide concise “SBAR” (Situation, Background, Assessment, Recommendation) reports to the remote supervisor, enabling the physician to make rapid, informed decisions regarding treatment.
3. Medication Administration and Equipment Proficiency
On-site professionals must be legally permitted and clinically trained to administer emergency medications, including epinephrine, antihistamines, beta-agonists, and intravenous fluids. This includes proficiency in:
- Correct dosage calculations and administration routes (e.g., intramuscular epinephrine for anaphylaxis).
- Operation of emergency equipment such as automated external defibrillators (AEDs) and oxygen delivery systems.
- Maintenance of “crash carts” or contrast reaction kits to ensure all medications are unexpired and immediately accessible.
State and Local Compliance Considerations
Compliance with virtual supervision is not determined solely by federal rules. State medical boards and nursing boards often have disparate definitions of “scope of practice” and “immediate availability.”
Varying Regional Requirements
Certain states may impose restrictions that limit the types of personnel (e.g., radiologic technologists vs. registered nurses) permitted to administer medications or manage reactions under virtual supervision. For example, some jurisdictions may require a “licensed practitioner” (such as a PA or NP) to be on-site, even if a radiologist is available virtually. Administrators must conduct thorough legal reviews of state-specific statutes, such as those in Ohio or California, which have recently seen legislative activity regarding imaging supervision.
Documentation and Audit Readiness
Proper documentation is the primary defense during regulatory inspections or accreditation reviews. Facilities must maintain detailed logs that include:
- Evidence of real-time supervision for every contrast-enhanced study.
- Records of staff competency assessments and “mock code” training dates.
- Logs of technology system checks and uptime percentages.
- Incident reports for any adverse reactions, detailing the response time of the remote physician.
Operational Benefits for Radiology Departments
Transitioning to a virtual supervision model allows radiology departments to address physician shortages and optimize workflow. By centralizing supervision, a single radiologist can provide oversight for multiple satellite facilities, reducing the need for on-site physician coverage in low-volume centers or rural areas.
This model also enhances scheduling flexibility. Facilities can extend their operating hours into evenings and weekends without the overhead of an on-site radiologist, improving patient access and reducing the backlog for diagnostic imaging. Furthermore, virtual supervision provides a reliable backup system for unexpected physician absences, ensuring that patient scans are not canceled due to a lack of on-site oversight.
Implementation and the Role of Expert Training
Successful adoption of virtual supervision requires more than just a software installation; it necessitates the integration of technology with clinical training. ContrastConnect emphasizes that the efficacy of the remote supervisor is directly linked to the proficiency of the on-site team. By combining high-fidelity virtual supervision platforms with expert-led, on-site reaction management training, radiology departments can bridge the gap between regulatory requirements and operational reality.
The future of diagnostic imaging is defined by this hybrid approach—leveraging the reach of telecommunication while grounding the practice in traditional clinical safety.
ContrastConnect
Las vegas
Las Vegas
NV
89109
United States